BASH Guideline
Section 1: The Clinical Approach
Section 2: Primary Headaches

2.4 The trigeminal autonomic cephalalgias
2.4.1 Cluster headache
2.4.1.1 Epidemiology
Cluster headache has a prevalence of about 0.1% (Fischera et al., 2008).
The peak age of onset is between the 3rd and 4th decades (Ekbom, 1970b; Friedman & Mikropoulos, 1958; Kudrow, 1980; Manzoni et al., 2016; Sutherland & Eadie, 1972; Vikelis & Rapoport, 2016)
The disorder is four times more common in men (Fischera et al., 2008).
Cluster headache sufferers are often smokers (Manzoni, 1999; Sjaastad, 1992; Vikelis & Rapoport, 2016).
2.4.1.2 Clinical features
The current classification of cluster headache is well validated (http://www.ichd- 3.org).
Attacks are characterised by excruciating and strictly unilateral headache. However, attacks can change side, across different bouts, within the same bout and rarely within an acute attack (Ekbom, 1970a; Friedman & Mikropoulos, 1958; Kudrow, 1980; Lance & Anthony, 1971; Schurks et al., 2006; Sutherland & Eadie, 1972; Torelli et al., 2001).
Bilateral pain in cluster headache is rare (Donnet et al., 2007; Kudrow, 1980; Sjaastad et al., 1985; Vikelis & Rapoport, 2016; Young & Rozen, 1999).
The attacks are accompanied by ipsilateral cranial autonomic features which are primarily parasympathetic and can most commonly include lacrimation, conjunctival injection, rhinorrhoea, nasal congestion, drooping or swelling of the eyelid. The presence of cranial autonomic features in headache does not necessarily indicate cluster headache or another TAC. For example, these features can also occur in migraine.
One of the most distinguishing features during the cluster attack is restlessness. Patients typically walk up and down, or rock to and fro, clutching the affected side, unlike migraineurs who are motion-sensitive and prefer to remain still (Bahra et al., 2002; Schurks et al., 2006; Torelli et al., 2001; Vikelis & Rapoport, 2016).
Attack duration is usually between 15 minutes to 3 hours and attack frequency 1-2 a day. Cluster headache can be episodic or chronic. Episodic cluster bouts usually last between 2 weeks and 3 months and most often occur once every 1-2 years. Ten to 20% of sufferers experience chronic cluster headache, which is currently defined as attacks occurring without a remission period, or with remissions lasting < 3 month, for at least 1 year (Bahra et al., 2002; Ekbom, 1970a; Friedman & Mikropoulos, 1958; Kudrow, 1980; Lance & Anthony, 1971; Schurks et al., 2006; Sutherland & Eadie, 1972).
Active bouts of cluster headache can be seasonal and at the same time each year. During an active bout, sufferers can experience attacks at set times during the day for weeks or months. The pattern can change or become less predictable (Friedman & Mikropoulos, 1958; Hornabrook, 1964; Kudrow, 1987; Sutherland & Eadie, 1972; van Vliet et al., 2006; Vikelis & Rapoport, 2016).
Cluster attacks often wake patients from sleep, usually about 1.5-2 hours after they have fallen asleep (Bahra et al., 2002; Barloese et al., 2015; Ekbom, 1970a; Russell, 1981; Vikelis & Rapoport, 2016).
Some individuals can exclusively have nocturnal attacks (Ekbom, 1970a).
In between attacks of pain patients can experience a background dull ache in the same distribution of the cluster attacks. The interparoxysmal pain tends to settle when the cluster bout resolves (Marmura et al., 2010).
During an active cluster bout some patients can be exquisitely sensitive to alcohol triggering an attack, usually within an hour. The propensity does not occur out of the bout (Ekbom, 1968).
Clinically relevant commonalities and differences between migraine and cluster headache include:
- Cluster sufferers can have nausea and vomiting, photophobia and phonophobia (Bahra et al., 2002; Schurks et al., 2006; Torelli et al., 2001; Vikelis & Rapoport, 2016)
- Up to 25% of migraine sufferers can experience autonomic features during an attack (Ekbom, 1970a)
- Aura can be experienced in up to 23% of cluster headache sufferers (Bahra et al., 2002; Donnet et al., 2007; Rozen & Fishman, 2012; Schurks et al., 2006) (though in practice is rare)
- 20-40% of migraine sufferers experience strictly unilateral headache (D'Amico et al., 1994; Kelman, 2005)
- The duration of untreated migraine attacks in adults is invariably longer than 4 hours (Davies et al., 1991; Kelman, 2006)
- A key feature in cluster headache is restlessness and lack of motion sensitivity, while migraine sufferers prefer to be still (Bahra et al., 2002; Schurks et al., 2006; Torelli et al., 2001; Vikelis & Rapoport, 2016)
2.4.1.3 Management
A) Acute Treatment
The most effective acute treatment is the sumatriptan 6mg subcutaneous injection with significant relief within 15 minutes (Ekbom & Group, 1991).
The maximum limit is two 6mg injections a day (Ekbom & Cole, 1993).
The treatment is generally well tolerated, without tachyphylaxis (Ekbom et al., 1995; Gobel et al., 1998).
Patients who have cluster headache rarely develop medication overuse headache (Ekbom et al., 1995; Gobel et al., 1998).
Patients who also have migraine may develop exacerbation of their migraine disorder whilst using a triptan effectively for their cluster attacks (Hering-Hanit, 2000; Paemeleire et al., 2006).
High flow oxygen 100% at 7-15 litres/minute for 15-20 minutes, using a non-rebreathable mask, is effective in aborting acute attacks of cluster headache (Cohen et al., 2009; Fogan, 1985).
There is no limit to the use of high flow oxygen, though obvious cautions around smoking/flames/fire hazards near oxygen need to be considered/addressed. Oxygen is often used together with triptans in patients with multiple attacks. Table 10 shows recommended acute cluster attack treatments.
Table 1. Recommended Acute Cluster attack treatments
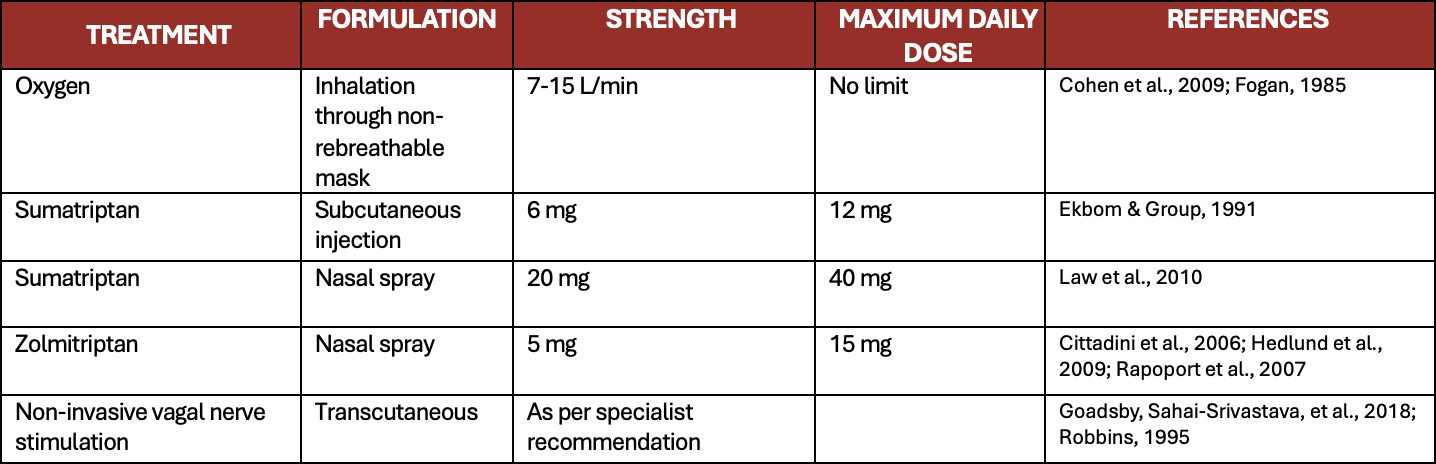
B) Preventive treatments
Verapamil is an effective preventive treatment in cluster headache (Leone et al., 2000).
The doses required to suppress cluster headache attacks can be higher than those used to treat cardiac disorders. Clinically significant cardiac rhythm disturbances can occur and are neither dose nor time dependent (Cohen et al., 2007; Lanteri-Minet et al., 2011). It is possible for patients to develop cardiac conduction abnormalities even after they have been on a stable dose for a long period.
BASH recommends an ECG done at baseline and following each increase in dose. At a stable dose ECG should be done once every six months. Any cardiac rhythm disturbance may require dose reduction or drug withdrawal (Cohen et al., 2007).
In episodic cluster headache, once control has been achieved, towards the end of the expected bout, the preventive can be slowly withdrawn. If attacks recur the preventive should be re-established.
Oral corticosteroids have been shown to be effective in the prevention of cluster headache attacks (Jammes, 1975).
The response should be seen within 48 hours. Given the high adverse effect profile corticosteroid use is best restricted as a short-term measure in patients with multiple daily attacks, which cannot be treated effectively acutely, whilst an alternative preventive is being introduced.
Suboccipital nerve block (i.e. suboccipital depot steroid and local anaesthetic injection) has shown a significant reduction or resolution of attacks compared to placebo and despite a high placebo response rate (Ambrosini et al., 2005; Leroux et al., 2011).
Table 2 shows recommended preventive treatments for cluster headache.
Table 2: Recommended preventive treatments for cluster headaches
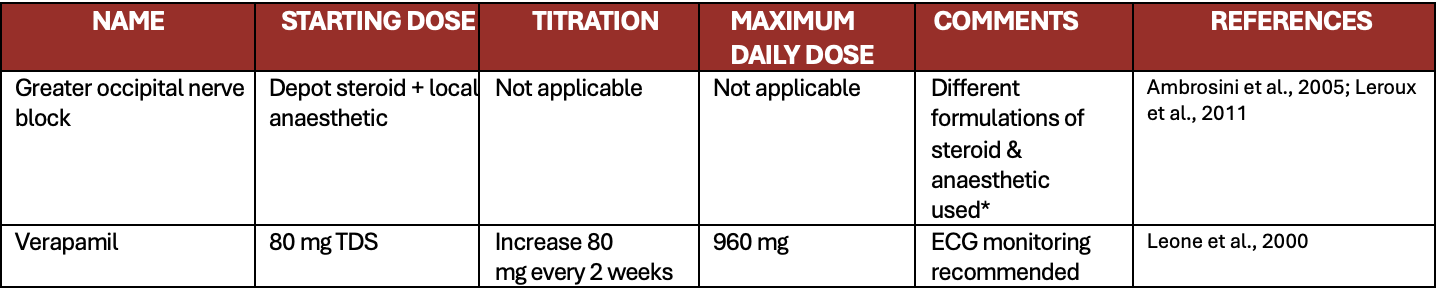
*There does not seem to be a difference between different local anaesthetics
Appendix 1: All acute cluster attack treatment
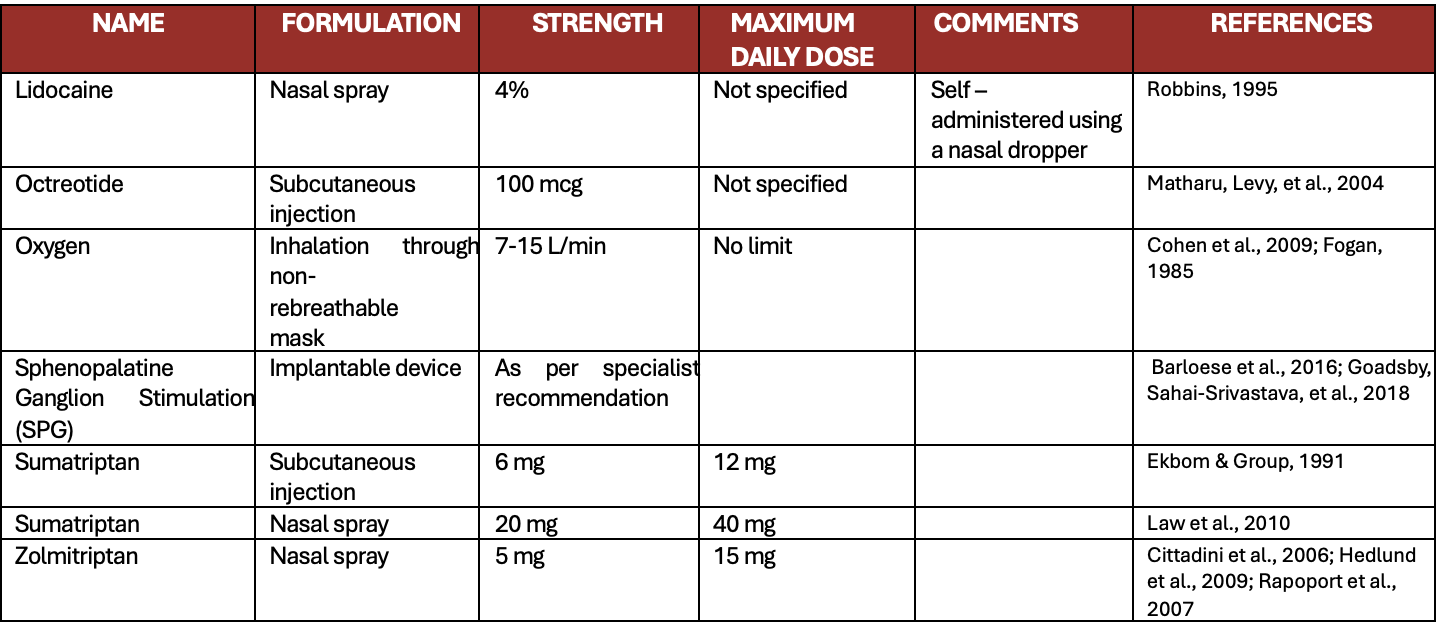
Appendix 2: All preventive treatments for cluster headaches
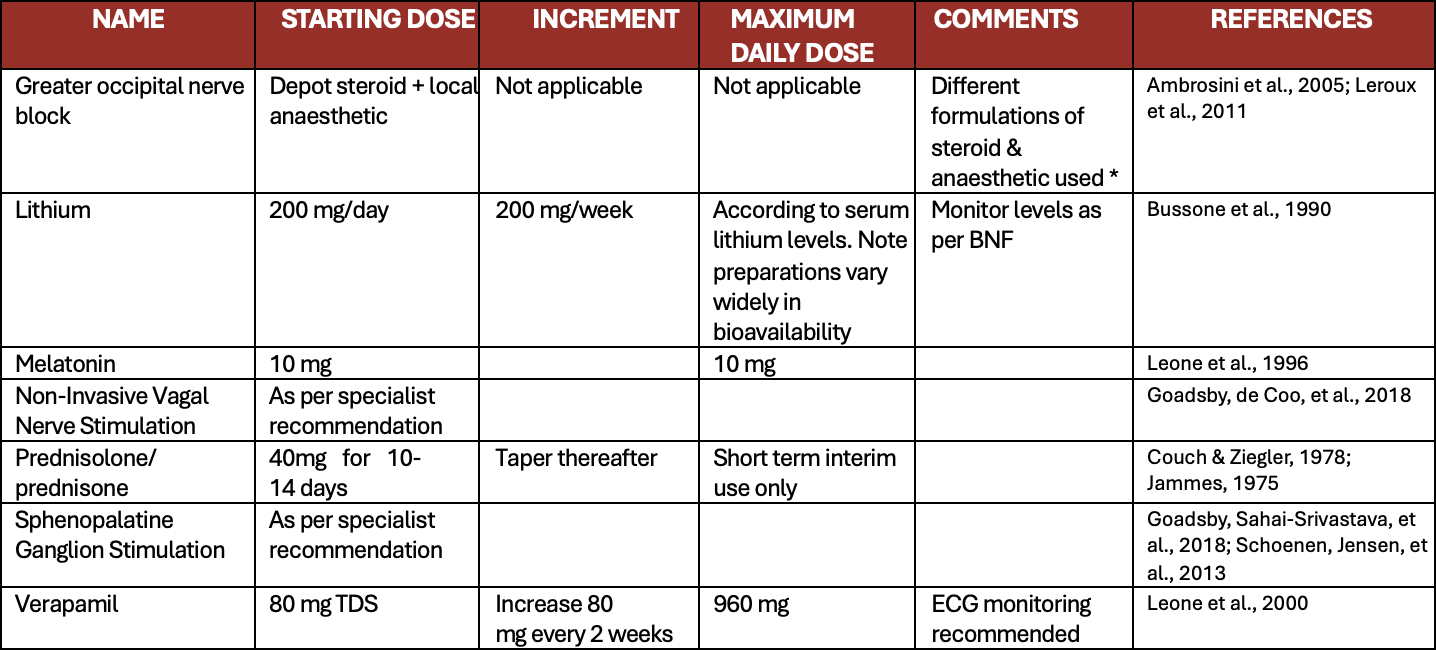
*There does not seem to be a difference between different local anaesthetics
Appendix 3: Classification of cluster headache (http://www.ichd-3.org)

