BASH Guideline
Section 1: The Clinical Approach
Section 2: Primary Headaches

2.4 The trigeminal autonomic cephalalgias
2.4.4. Hemicrania continua
2.4.4.1 Epidemiology
Hemicrania continua is an uncommon disorder with estimated prevalence of 0.8-1.5% however it is acknowledged that this is compounded by diagnostic inaccuracy (Bigal, Lipton et al., 2004; Ramon et al., 2013).
The disorder seems to be more common in women. Mean age of onset is between the 3rd and 4th decade (Cortijo et al., 2012; Peres et al., 2001).
*The paroxysmal trigeminal autonomic cephalalgias can have pain between acute attacks. In most cases the interparoxysmal pain is part of the same disorder. In some cases, hemicrania continua may be co-exist. Therefore, a trial of Indomethacin could be considered (Cosentino et al., 2010; Robbins et al., 2010; Totzeck et al., 2014)
2.4.4.2 Clinical features
Hemicrania continua is characterised by strictly unilateral pain of moderate severity with ipsilateral autonomic features which may be more prominent during exacerbations.
Hemicrania continua has both clinical and pathophysiological overlap with migraine (Matharu, Cohen, et al., 2004)
Thus, although more than half of cases can be restless during the attacks, others experience motion sensitivity (Cittadini & Goadsby, 2010; Cortijo et al., 2012; Newman et al., 1994; Peres et al., 2001; Prakash & Golwala, 2012).
Although the disorder is defined by chronicity it can present in a relapsing and remitting (thus episodic) form (Joubert, 1991; Kuhn et al., 2005; Pareja, 1995; Peres et al., 2001; Terlizzi et al., 2011; Yablon & Newman, 2010).
2.4.4.3 Management
There are no RCTs for preventive treatment in hemicrania continua.
A) Acute treatment
Medication overuse can occur in hemicrania continua. Thus, analgesics should be withdrawn prior to assessing response to indomethacin (Weatherall & Bahra, 2011; Young & Silberstein, 1993).
B) Preventive treatment
Hemicrania continua is an indomethacin-sensitive disorder. The effective dose range is between 25-300mg daily dose (Antonaci & Sjaastad, 1989; Boes & Dodick, 2002; Cittadini et al., 2008; Prakash et al., 2013).
Although most patients show a rapid response to Indomethacin, some patients can take up to a week to demonstrate a response to an effective dose. Based upon this BASH recommends Indomethacin 25mg TDS for 7 days, 50mg TDS 7 days, up to 75mg TDS.
Dose requirements can change over time and some patients may go into remission (Pareja et al., 2001).
Therefore, once symptoms are well controlled for a period of time gradual dose reduction should be tried to maintain the lowest effective dose or, if there is no recurrence on each dose reduction, withdrawal during remission periods.
Gastrointestinal side effects with Indomethacin are common and may preclude use of the drug. A concomitant proton-pump blocker or H2-antagonist can be used.
Appendix 1. Classification of hemicrania continua (http://www.ichd-3.org)

Appendix 2. Differential diagnosis of The Trigeminal Autonomic Cephalalgias and Trigeminal Neuralgia
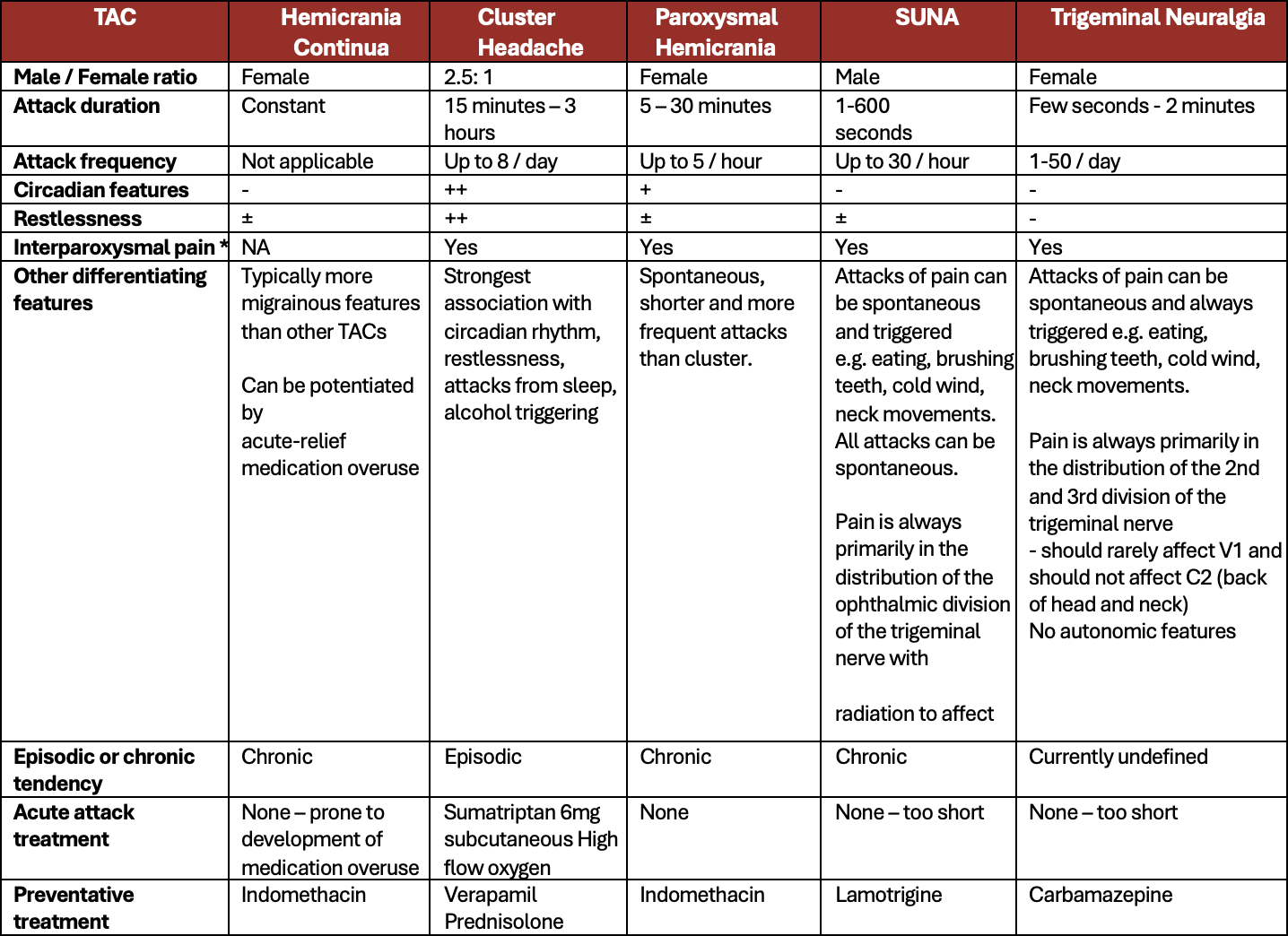
*The paroxysmal trigeminal autonomic cephalalgias can have pain between acute attacks. In most cases the interparoxysmal pain is part of the same disorder. In some cases, hemicrania continua may be co-exist. Therefore, a trial of Indomethacin could be considered (Cosentino et al., 2010; Robbins et al., 2010; Totzeck et al., 2014)
