BASH Guideline
Section 1: The Clinical Approach
Section 2: Primary Headaches

1.1 Clinical assessment of headache
1.1.1 Classification
Headaches are classified by the International Headache Society as primary or secondary headaches (http://www.ichd-3.org).
The majority of headache is primary (such as migraine). Primary headache is the best validated within this classification system (http://www.ichd-3.org).
Secondary headaches are precipitated by another condition or disorder, local or systemic (Katzman et al., 1999; Morris et al., 2009; Vernooij et al., 2007). Serious causes of secondary headache are uncommon.
1.1.2 How to differentiate primary from secondary headache
The most consistent indicators for serious secondary headache are:
- Thunderclap (sudden onset) headache (Landtblom et al., 2002; Linn et al., 1998; Locker et al., 2006)
- Associated focal neurological deficit (Hamilton & Kernick, 2007; Locker et al., 2006; Sempere et al., 2005)
- Associated systemic features (Hamilton & Kernick, 2007; Locker et al., 2006; Sempere et al., 2005)
- Patients over the age over 50 years (Edlow et al., 2008; Ramirez-Lassepas et al., 1997)
The history is the key to diagnosis in headache. The neurological examination is also helpful in differentiating primary from secondary headache (Hamilton & Kernick, 2007; Locker et al., 2006; Sempere et al., 2005). For example, patients with migraine (with or without typical aura) or tension-type headache and a normal neurological examination do not have an increased likelihood of a secondary precipitant relative to the background population (Alter et al., 1994; Kernick et al., 2008; Kurth et al., 2015).
For other isolated headache syndromes with normal neurological examination there is insufficient data to enable a definitive conclusion (Ontario, 2010).
1.1.3 Using the temporal pattern of headache to help differentiate primary from secondary headache
While we acknowledge that not all the following descriptors have tight definitions, we have tried to consider different temporal clinical patterns that the ‘jobbing’ clinician might frequently encounter and recognise.
Sudden onset headache
Sudden onset headache reaching maximum intensity within 5 minutes is called thunderclap headache (Aygun & Bildik, 2003; Landtblom et al., 2002; Linn et al., 1998; Locker et al., 2006; Physicians, 2002; Shibata et al., 2006). Thunderclap headache has the greatest probability of a secondary precipitant (Landtblom et al., 2002; Linn et al., 1998; Locker et al., 2006).
Recent onset and progressive headache
Evolution of headache over days to weeks. If associated systemic features and/or focal neurological signs there is an increased probability of secondary precipitant (Hamilton & Kernick, 2007; Locker et al., 2006; Sempere et al., 2005).
Recurrent episodic headache
Recurrent episodic headache in isolation is most likely due to a primary headache disorder (Alter et al., 1994; Tsushima & Endo, 2005).
Headache which occurs on the majority of days in a month
Headache present for at least 15 days per month for over 3 months in isolation is most likely due to a primary headache disorder (Tsushima & Endo, 2005).
1.1.4 Differentiating between common primary headache disorders
Laterality and site of headache
Strictly unilateral (right or left but never bilateral) headache most consistently occurs in the Trigeminal Autonomic Cephalalgias (TACS) (http://www.ichd-3.org). 11.5 - 20% of migraine sufferers experience unilateral headache (D'Amico et al., 1994; Momoh-Ojewuyi et al., 2013).
Bilateral headache more commonly occurs in migraine and is a more consistent defining feature of tension-type headache (Iversen et al., 1990; Lance & Anthony, 1966; Rasmussen et al., 1991).
In most primary headache disorders the pain is experienced in the distribution of the first division of the trigeminal nerve and second cervical root. Neck pain can therefore be a feature of a migraine attack (Bahra et al., 2000; Cittadini & Goadsby, 2010; Cittadini et al., 2008; Cohen et al., 2006; Iversen et al., 1990; Kelman, 2005; Prakash et al., 2013; Torelli et al., 2001; Vikelis & Rapoport, 2016).
Associated symptoms
Prominent features in migraine include nausea, vomiting, photophobia, phonophobia and motion sensitivity (a tendency for the headache to be exacerbated by head movement or mild exertion) (Blau & Dexter, 1981; Davies et al., 1991; Lance & Anthony, 1966; Olesen, 1978; Rasmussen et al., 1991; Russell et al., 1996).
Cranial autonomic features, such as lacrimation, conjunctival injection, rhinorrhoea, and nasal blockage, are characteristic of the TACs, but studies reported cranial autonomic symptoms occurring in 26% to 80% of migraine sufferers (Ekbom, 1970a; Obermann et al., 2007; Tiwari et al., 2022)).
Unlike migraine sufferers who are frequently motion sensitive and generally prefer to remain still during an attack, patients with cluster headache and to a lesser extent TACs tend to be restless during an attack (Bahra et al., 2000; Schurks et al., 2006; Torelli et al., 2001; Vikelis & Rapoport, 2016)
Aura can be experienced in all headache disorders, but is by far most common in migraine (Krymchantowski, 2005).
Duration and Frequency
The majority of untreated migraine headaches last between 4-72 hours (Kelman, 2006; Russell et al., 1996; Selby & Lance, 1960).
Untreated TACS are typically of shorter duration and with higher attack frequency (Bahra et al., 2002; Boes & Dodick, 2002; Kudrow, 1980; Manzoni, 1999; Prakash & Patell, 2014; Sjaastad et al., 1989; van Vliet et al., 2006; Weng et al., 2017).
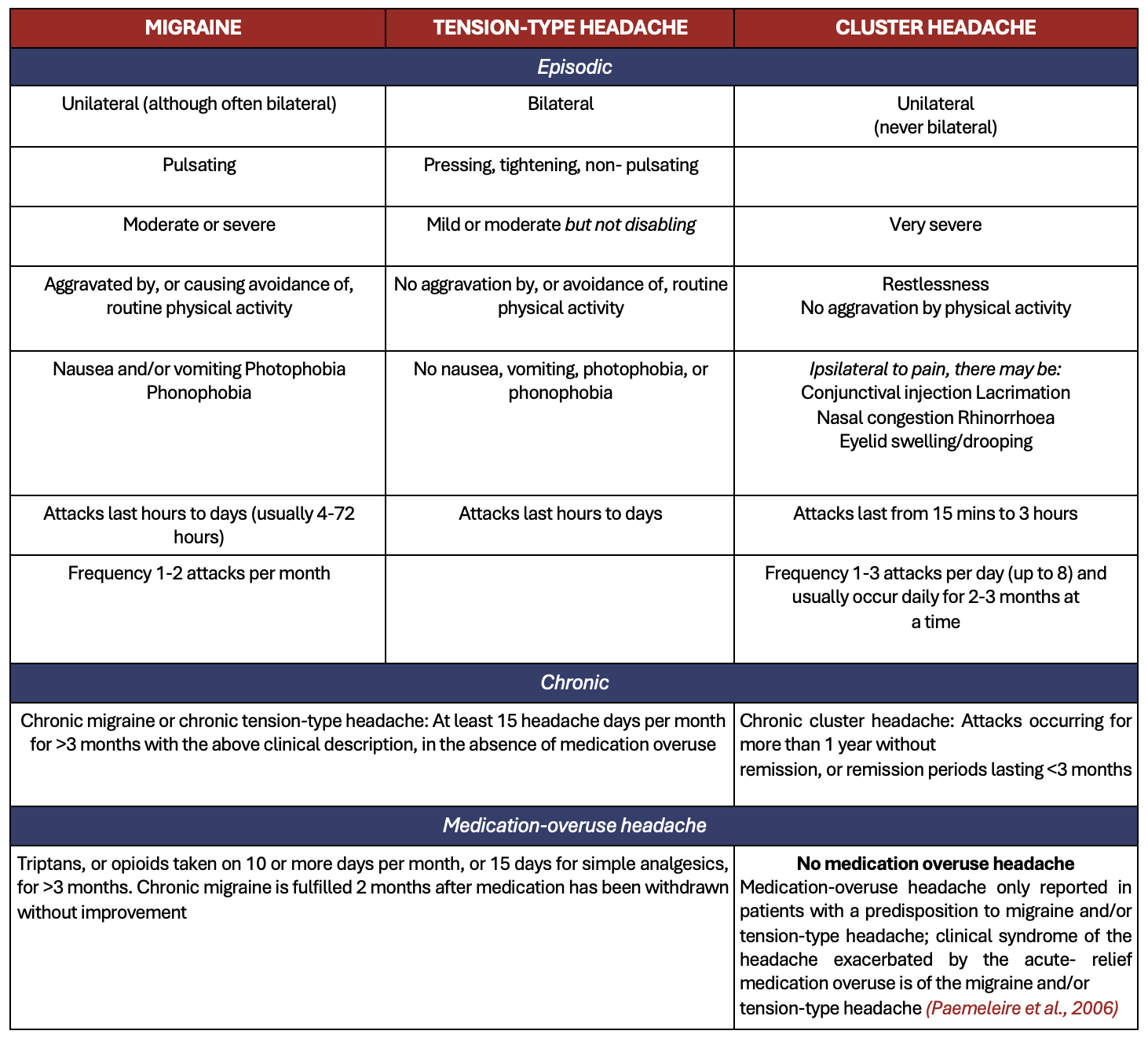
Table 1 shows a comparative table to distinguish between common primary headaches.
Table 1: Comparative table to distinguish between common primary headaches (based on http://www.ichd-3.org)
1.1.5 Examination
The presence of abnormal neurological signs significantly increases the chance of an intracranial abnormality. Therefore, an appropriate neurological examination including fundoscopy is required when assessing the patient presenting with headache.
Useful and brief ways to perform the neurological examination are found at:
